
Bad Signs After ACL Surgery: A Complete Guide to Recognizing and Managing Complications
Reviewed by: Dr. James Morrison, MD, FAAOS | Board-Certified Orthopedic Surgeon
ACL surgery is one of the most common orthopedic procedures performed worldwide, with over 200,000 reconstructions carried out in the United States alone each year. Most patients follow a predictable recovery arc: swelling, stiffness, physiotherapy, and a gradual return to activity. But for some patients, recovery takes an unexpected turn, and knowing the bad signs after ACL surgery can make the difference between a swift intervention and a serious, lasting setback.
The challenge is that many ACL surgery complications can mimic normal post-operative symptoms in their early stages. A wound that looks slightly red may be normal irritation or the beginning of a deep infection. Persistent swelling may be routine healing or an early indicator of a blood clot. Pain that is not improving may reflect expected tissue remodelling or graft failure. Without a clear framework, it is genuinely difficult for patients to know what warrants a phone call to their surgeon and what can safely wait until the next appointment.
This guide gives you that framework. It covers every significant bad sign after ACL surgery in plain language, explains why each happens, and tells you exactly how urgently to act. Whether you are one week or three months post-operation, understanding the warning signs of ACL surgery complications could protect your knee and your recovery. For a broader look at how the body recovers from major orthopaedic events, see how to speed up recovery from a traumatic injury on Doctiplus.com.
Normal Recovery vs. Bad Signs After ACL Surgery
Before identifying what is wrong, it helps to know what is right. The first two weeks after ACL reconstruction involve significant inflammation, bruising, and discomfort. These are expected and do not indicate a problem. The table below draws a clear line between what is normal and what represents a bad sign after ACL surgery that requires attention.
| Days 1 to 3 | Swelling, bruising, moderate pain, warmth around the knee | Fever above 38.5C, excessive bleeding through dressings, numbness in foot or toes |
| Days 4 to 14 | Gradual reduction in swelling, wound closure, improving range of motion | Increasing redness or discharge from wound, calf swelling or pain, sudden sharp knee pain |
| Weeks 2 to 6 | Some stiffness, aching after physio sessions, occasional swelling with activity | Wound that will not close, persistent fever, knee locked in position, signs of DVT |
| Months 2 to 6 | Gradual strength improvements, mild soreness with new exercises, some clicking | Sudden giving way of the knee, return of original injury feeling, no strength progress |
Bookmark this table and refer to it whenever you are unsure whether a symptom is expected. When in doubt, contact your surgical team. The Mayo Clinic advises patients to call their surgeon immediately for fever, increasing pain not controlled by medication, signs of infection, or calf pain and swelling.
Signs of Infection After ACL Surgery
Infection is one of the most serious signs after ACL surgery. It affects approximately 0.3 to 1.7 percent of ACL reconstructions according to research published in the American Journal of Sports Medicine, but the consequences can be severe, including graft loss and chronic joint damage if not caught early.
Superficial Wound Infection
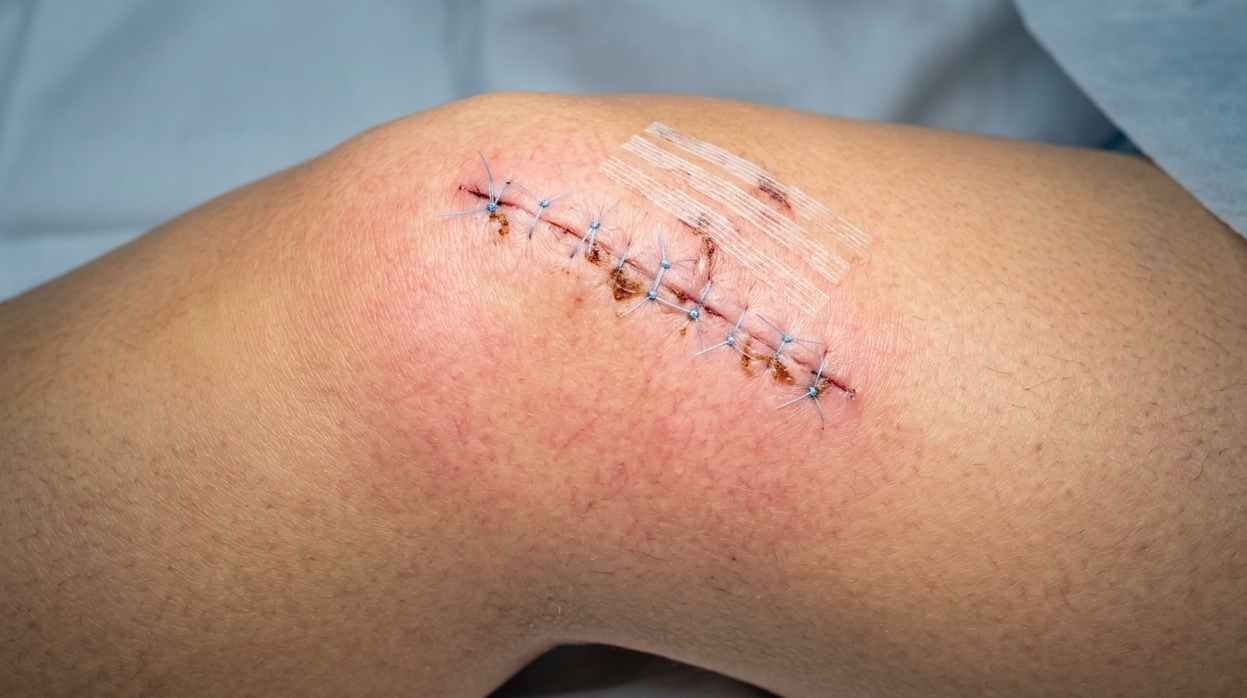
A superficial infection involves the skin and tissue immediately around the incision. Signs include:
- Redness that spreads beyond the wound edge and worsens after day three
- Warmth that is noticeably greater than the surrounding skin
- Yellow, green, or foul-smelling discharge from the incision
- Wound edges that pull apart or fail to close
- Fever above 38.0 degrees Celsius
Superficial infections are typically treated with oral antibiotics and do not necessarily threaten the graft, but they must be treated promptly to prevent spread.
Deep or Septic Arthritis
A deep joint infection, or septic arthritis, is a far more serious complication and a severe sign after ACL surgery. The knee becomes a contained environment where bacteria can multiply rapidly, destroying cartilage and the graft itself within days. Symptoms include:
- High fever (above 38.5 °C) that does not respond to paracetamol or ibuprofen
- A knee that is hot, red, and extremely swollen, often more than it was immediately post-surgery
- Severe, worsening pain that is no longer manageable with prescribed pain relief
- General systemic illness, including chills, rigors, or feeling severely unwell
Septic arthritis after ACL reconstruction is a surgical emergency. The Cleveland Clinic confirms that without prompt joint washout and intravenous antibiotics, permanent joint destruction occurs. If you suspect deep infection, go to the emergency department rather than waiting for a routine appointment.
Deep Vein Thrombosis: A Dangerous Bad Sign After ACL Surgery
Deep vein thrombosis (DVT), a blood clot forming in the deep veins of the leg, is a well-documented ACL surgery complication. Studies cited by the NHS indicate that orthopaedic surgery significantly elevates DVT risk due to reduced mobility, surgical trauma, and tourniquet use during the procedure.
The classic signs of DVT after ACL surgery include:
- Calf pain or tenderness, often described as a cramp that does not resolve.
- Noticeable swelling in the calf, ankle, or foot that is one-sided and worsening
- Skin in the affected leg that is red, warm to the touch, or discoloured
- Feeling of heaviness or tightness in the lower leg
The critical concern with DVT is pulmonary embolism (PE), where the clot breaks off and travels to the lungs. Signs of PE include sudden breathlessness, chest pain, rapid heart rate, or coughing up blood. This is a life-threatening emergency requiring immediate attendance at an emergency department. If you notice any combination of leg swelling with breathing difficulty after ACL surgery, call emergency services without delay. For guidance on when urgent medical attention is appropriate, see When Immediate Medical Attention Is the Right Call on Doctiplus.com.
ACL Graft Failure: Signs Your Reconstruction May Not Be Holding
ACL graft failure is among the most disheartening signs after ACL surgery, and unfortunately, it is not rare. Research published in the British Journal of Sports Medicine estimates that re-rupture rates range from 6 to 25 percent depending on patient age, graft type, and return-to-sport timeline, with younger and more active patients at the highest risk.
Warning signs that the ACL graft may be failing or has failed include:
- Sudden giving way: The knee buckles unexpectedly during walking, pivoting, or returning to sport. This is the single most telling sign of graft failure.
- A pop or snap: A sensation or sound similar to the original ACL tear is highly significant and warrants same-day contact with your surgeon.
- Rapid swelling: Haemarthrosis, or blood pooling inside the joint, causes rapid, tense swelling within hours of an injury to the graft.
- Loss of stability: A feeling that the knee is loose, unreliable, or moving in a way it should not during activity or even at rest.
- No progression in strength: If quadriceps and hamstring strength have plateaued for more than four to six weeks despite consistent physiotherapy, the graft may not be integrating correctly.
ACL graft failure does not always mean a second reconstruction is required, but it always requires prompt evaluation. Continuing to load a failing graft risks further damage to the meniscus and cartilage. For patients also experiencing broader knee pain concerns, the Doctiplus article on non-surgical treatments for knee pain: what patients need to know provides a useful overview of conservative management options alongside surgical decisions.
Nerve Damage and Vascular Complications After ACL Surgery
Nerve Damage Signs
Nerve injury during ACL reconstruction most commonly affects the infrapatellar branch of the saphenous nerve, which runs near standard incision sites. The National Institutes of Health notes that minor sensory changes are common and usually temporary, but the following signs warrant investigation:
- Persistent numbness or tingling on the inner side of the knee or upper shin
- Sharp, shooting, or burning pain along the inner leg that worsens rather than improves
- Complete loss of sensation over a patch of skin that does not recover within four to six weeks
- Foot drop, meaning difficulty lifting the foot or toes, which suggests peroneal nerve involvement and is a more serious complication
Vascular Complications
Vascular injury after ACL surgery is rare but severe. Signs that suggest a vascular problem include:
- A foot or lower leg that is pale, cold, or blue compared to the other limb
- Absence of a pulse in the foot post-operatively
- Rapidly increasing swelling in the knee not explained by a normal haematoma.
- Severe, unrelenting pain that is disproportionate to the expected post-surgical course
Any sign of vascular compromise after ACL surgery requires immediate emergency evaluation. Limb loss is a real risk when arterial injury goes untreated.
Arthrofibrosis: When Stiffness Is a Bad Sign After ACL Surgery
Some degree of stiffness is expected after ACL reconstruction. Arthrofibrosis, however, is a pathological scarring response where excessive fibrous tissue forms inside the joint, severely limiting the range of motion. It affects an estimated 4 to 35 percent of ACL reconstructions, according to data reviewed by the American Academy of Orthopaedic Surgeons, with the wide range reflecting differences in surgical technique, rehabilitation timing, and individual biology.
Signs that stiffness has crossed the line into arthrofibrosis include:
- Inability to fully straighten the knee (extension deficit) beyond six weeks post-surgery
- Inability to bend the knee past 90 degrees despite regular physiotherapy
- A knee that feels mechanically blocked rather than simply tight or sore
- Persistent swelling and warmth in the absence of infection, lasting beyond four weeks
Early physiotherapy is the best prevention, which is why rehabilitation should begin within days of surgery. If arthrofibrosis is diagnosed, manipulation under anaesthesia or arthroscopic release may be required. For patients trying to understand the broader relationship between movement and recovery outcomes, the Doctiplus piece on the connection between movement and mental well-being is a helpful companion read.
Urgency Guide: What to Do When You Spot a Bad Sign After ACL Surgery
Not every complication requires the same response. Use this colour-coded urgency guide to decide your next step.
| RED: Emergency | Chest pain, breathlessness, suspected PE, signs of septic arthritis, vascular compromise (cold pale limb), foot drop | Call emergency services (999 or 112) or go to the emergency department immediately |
| AMBER: Urgent | DVT signs (calf swelling, warmth, one-sided), high fever, sudden giving way of the knee, rapidly increasing joint swelling, wound that is opening or heavily discharging | Contact your surgeon or orthopaedic team same day. If unavailable, attend urgent care |
| GREEN: Routine | Numbness around the incision, slow strength progress, mild persistent stiffness, minor wound redness without spreading, questions about recovery timeline | Raise at your next scheduled appointment or call the surgical team during business hours |
Mental Health After ACL Surgery: A Warning Sign Patients Often Miss

One of the least discussed bad signs after ACL surgery is the psychological toll of a long, unpredictable recovery. Research published in the Journal of Athletic Training found that clinically significant depression and anxiety affect 20 to 30 percent of ACL surgery patients during recovery, and that psychological readiness is one of the strongest predictors of successful return to sport.
Watch for these psychological warning signs:
- Persistent low mood, withdrawal from social activities, or loss of motivation lasting more than two weeks
- Excessive fear of re-injury that prevents engagement with physiotherapy exercises
- Disproportionate anger or frustration around recovery setbacks
- Sleep disruption linked to pain rumination or anxiety about the knee
These are not signs of weakness. They are recognised clinical complications of any major orthopaedic surgery. Raising them with your surgical team opens the door to psychology referrals, which the evidence shows meaningfully improve both mental and physical recovery outcomes. For patients also navigating lifestyle factors that affect healing,
The Doctiplus guide on why modern lifestyles are leaving us nutrient-deficient explores how nutritional status interacts with the body’s capacity to repair tissue after surgery.
Daily Self-Check Routine for ACL Recovery
Run through this five-point check each morning during the first six weeks of your ACL recovery. It takes under two minutes and helps you catch bad signs before they escalate.
| 1 | Wound appearance | Dry, closed, fading pink | Redness spreading, discharge, swelling at incision |
| 2 | Swelling level | Gradually reducing week on week | Sudden increase, tense joint, rapid balloon-like filling |
| 3 | Temperature | No fever; warm knee is normal early on | Fever above 38.0C, or knee dramatically hotter than other side |
| 4 | Calf and foot | Both legs feel symmetrical | One calf swollen, tender, warm, or foot pale and cold |
| 5 | Pain trajectory | Trending downward each week | Pain plateau or worsening despite compliance with rehab |
For patients recovering from other sports injuries alongside ACL repair, the Doctiplus overview of common sports injuries and how to prevent them provides a useful reference for understanding the full landscape of orthopaedic recovery.
“The patients who do best after ACL reconstruction are those who stay alert without becoming anxious. Knowing the genuine warning signs gives them the confidence to act decisively when something is wrong, and the reassurance to stay the course when recovery is simply being slow,” says Dr. James Morrison, MD, FAAOS, Board-Certified Orthopedic Surgeon.
Frequently Asked Questions
What are the most serious bad signs after ACL surgery?
The most serious bad signs after ACL surgery are symptoms of deep joint infection (septic arthritis), deep vein thrombosis, pulmonary embolism, vascular compromise, and ACL graft failure. Any combination of high fever, rapidly worsening pain, one-sided calf swelling, breathlessness, or sudden knee instability should trigger immediate contact with a medical professional.
How do I know if my ACL graft has failed?
The primary signs of ACL graft failure are a sudden giving way of the knee during activity, a pop or snap similar to the original injury, rapid swelling inside the joint, and a persistent feeling that the knee is loose or unreliable. These symptoms should be reported to your surgeon the same day they occur.
What does an infection look like after ACL surgery?
Infection after ACL surgery presents as spreading redness around the wound, increased warmth, yellow or green discharge, wound edges that reopen, and fever. A superficial infection may appear within the first week. Deep joint infection can develop later and involves a dramatically swollen, hot, painful knee alongside systemic illness such as chills and high fever.
Is it normal to have knee swelling months after ACL surgery?
Mild swelling after activity is normal for up to six months after ACL reconstruction. However, sudden or rapidly increasing swelling, swelling that is accompanied by warmth and pain, or swelling that appears after minimal activity and does not reduce with rest and elevation, warrants assessment by your surgical team.
When should I go to the emergency department after ACL surgery?
Go to the emergency department immediately if you experience any of the following: breathlessness or chest pain (possible pulmonary embolism), signs of vascular compromise such as a cold, pale limb, severe, uncontrolled pain, or symptoms of deep joint infection, including high fever and an extremely hot, swollen knee. For a broader guide on recognising when emergency care is appropriate, see When Immediate Medical Attention Is the Right Call on Doctiplus.com.
Can I prevent complications after ACL surgery?
Many ACL surgery complications are preventable with early physiotherapy, consistent use of prescribed compression and elevation, not returning to sport before being medically cleared, taking blood thinners if prescribed, and attending all follow-up appointments. Staying well nourished and hydrated also supports tissue healing and immune function.
How long does ACL recovery take?
Full recovery from ACL reconstruction typically takes 9 to 12 months before return to competitive sport, though bone-to-bone healing of the graft occurs within 12 to 16 weeks. The graft then undergoes a process called ligamentisation that takes many months. Athletes who return too early face significantly higher re-rupture rates. For guidance on managing the extended recovery from major orthopaedic procedures, the Doctiplus article on recognising failed back surgery symptoms that need a revision procedure offers a parallel perspective on monitoring post-surgical progress across different orthopaedic procedures.
Conclusion
Recognising the bad signs after ACL surgery is one of the most important skills a patient can develop during recovery. From infection and blood clots to graft failure and psychological distress, the complications that derail ACL recoveries are rarely subtle if you know what to look for. The urgency framework, daily self-check table, and symptom guide in this article give you the tools to monitor your own recovery with confidence.
Act quickly when red-tier symptoms appear. Raise amber-tier concerns the same day. And never dismiss a gut feeling that something is not right. Early intervention consistently leads to better outcomes than delayed action, regardless of which bad sign after ACL surgery you are dealing with. If you are also navigating chronic joint issues alongside your ACL recovery, the Doctiplus guide on arthritis and medical cannabis: can UK patients get a prescription provides relevant context on managing long-term joint conditions.
Medical Disclaimer
Medical Disclaimer: The information provided in this article is for educational purposes only and is not intended as medical advice. Always consult a qualified healthcare professional before making any decisions about your health, diagnosis, or treatment. Doctiplus does not endorse any specific treatments, procedures, or products mentioned in this article.
References
- Mayo Clinic. ACL Reconstruction: What You Can Expect. MayoClinic.org.
- NHS. Deep Vein Thrombosis (DVT). NHS.uk.
- Cleveland Clinic. Septic Arthritis. ClevelandClinic.org.
- American Academy of Orthopaedic Surgeons. Anterior Cruciate Ligament (ACL) Injuries. AAOS.org.
- National Institutes of Health. Infrapatellar Saphenous Nerve Injury After ACL Surgery. NCBI.nlm.nih.gov.
- Ardern C.L. et al. (2014). Return-to-Sport Outcomes After ACL Reconstruction Surgery. British Journal of Sports Medicine, 48(22).
- Nwachukwu B.U. Et al. (2019). Psychological Outcomes After ACL Reconstruction. Journal of Athletic Training, 54(4).



