
Menopause: What It Is, Stages, Age, Signs & Side Effects
Introduction
Menopause is a natural turning point in every woman’s life. the moment when the menstrual cycle permanently ends and the reproductive years come to a close. It is not a disease, but it does bring real physical and emotional changes that can affect daily life in meaningful ways. Understanding what menopause is, when it happens, and how to manage it can make this transition far less daunting. If your symptoms feel overwhelming at any point, a healthcare provider can help you find relief.
What Is Menopause?
Menopause is defined as the point in time when a woman has gone 12 consecutive months without a menstrual period. It marks the end of the ovaries’ regular release of eggs and their production of the hormones estrogen and progesterone. These two hormones play a central role in the menstrual cycle, pregnancy, bone health, heart function, and mood regulation.
- Menopause is confirmed only in hindsight after that full year of no periods has passed.
- The years leading up to it involve gradual hormonal changes, and many women feel the effects long before they reach that 12-month milestone.
- It can present as hot flashes, irregular periods, sleep disturbances, or mood shifts, among other changes.
Stages of Menopause
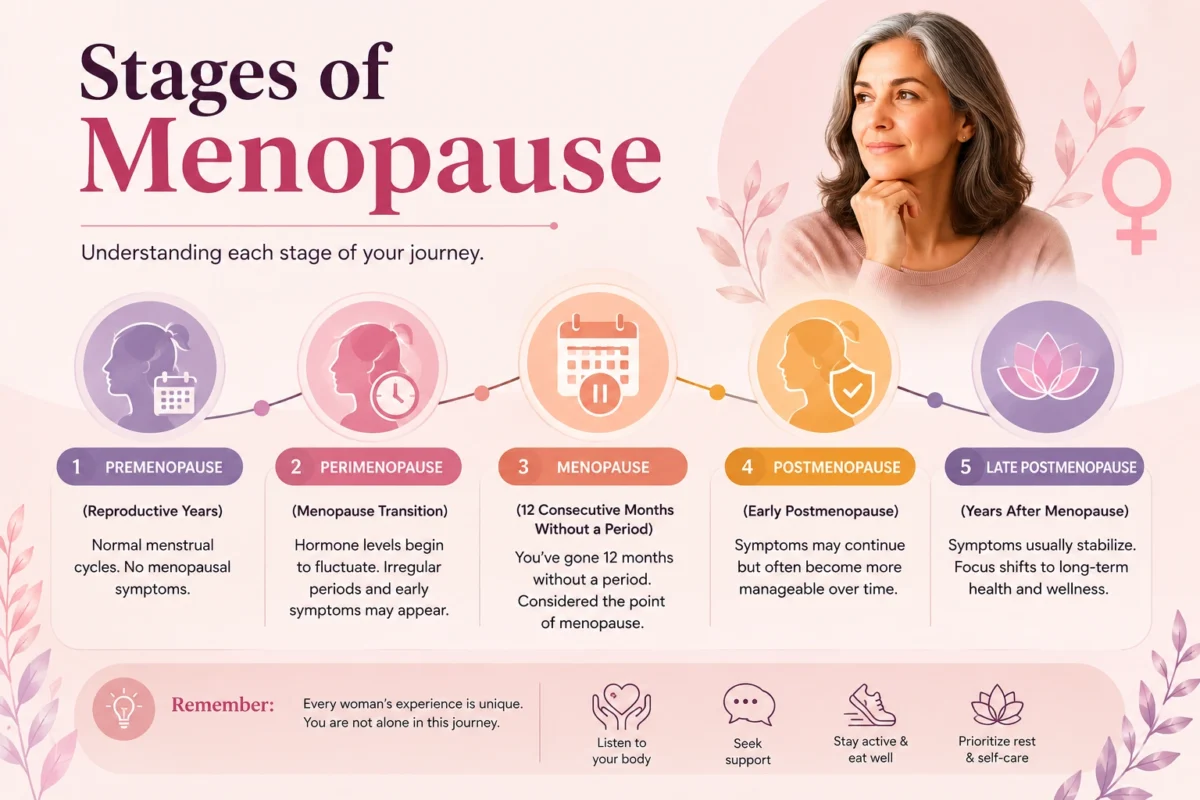
Menopause does not happen overnight. It unfolds in three distinct stages:
1. Perimenopause
This is the transitional phase that can begin in a woman’s early 40s or sometimes even her late 30s. Hormone levels start to fluctuate and decline. Periods may become irregular, heavier, or lighter. Many of the most recognized menopause symptoms, such as hot flashes and sleep problems, begin during perimenopause. This stage can last anywhere from a few months to more than a decade.
2. Menopause
Menopause itself is a single moment in time: the day that marks 12 full months without a menstrual period. Most women in the United States reach this point between the ages of 45 and 55, with the average age being around 51. At this stage, the ovaries have largely stopped producing estrogen and progesterone.
3. Postmenopause
This refers to all the years following menopause. Symptoms such as hot flashes and night sweats may ease over time, but low estrogen levels create long-term health considerations, particularly around bone density and cardiovascular health. Regular medical check-ups become especially important during this stage.
Possible Causes
Natural Causes
The most common cause of menopause is simply aging. As women get older, the ovaries gradually produce less estrogen and progesterone until they stop releasing eggs altogether. This natural process begins years before the final menstrual period.
Medical and Surgical Causes
In some cases, menopause occurs earlier or is brought on by medical intervention. These include:
Surgical menopause: Removal of both ovaries (oophorectomy) causes immediate menopause, regardless of age, because the main source of estrogen is removed.
Chemotherapy or radiation therapy: Cancer treatments can damage the ovaries and trigger premature menopause, sometimes temporarily and sometimes permanently.
Primary ovarian insufficiency (POI): Also called premature ovarian failure, this is when the ovaries stop functioning normally before age 40. It affects a small percentage of women and requires prompt medical evaluation.
Symptoms
Symptoms of menopause vary widely from woman to woman. Some experience only mild, manageable changes. Others find that symptoms significantly disrupt daily life. Common signs include:
Hot flashes: Sudden waves of warmth spreading across the face, neck, and chest, often accompanied by sweating and a flushed appearance. They can last from a few seconds to several minutes.
Night sweats: Hot flashes that occur during sleep, often causing soaked clothing and bedding, and disrupting rest.
Irregular or skipped periods: One of the earliest signs during perimenopause. Periods may become unpredictable before stopping altogether.
Vaginal dryness: Lower estrogen levels thin and dry the vaginal lining, which can cause discomfort, itching, and pain during sex.
Mood changes: Many women experience increased irritability, anxiety, or low mood, often linked to sleep disruption and hormonal shifts.
Sleep problems: Difficulty falling or staying asleep is common and is often made worse by night sweats.
Memory and focus issues: Some women notice forgetfulness or difficulty concentrating, sometimes called ‘brain fog.’
Decreased libido: A reduced interest in sex is common and is often tied to hormonal changes and vaginal discomfort.
Weight changes and slower metabolism: Hormonal shifts can lead to weight gain, particularly around the abdomen.
Thinning hair and dry skin: Lower hormone levels can affect the texture and fullness of hair and the moisture of the skin.
Diagnosis
For most women, menopause is diagnosed based on symptoms and menstrual history alone. If a woman is in her late 40s or early 50s, has been experiencing hot flashes and irregular periods, and has not had a period for 12 consecutive months, a clinical diagnosis can typically be made without further testing.
When symptoms appear early or the diagnosis is unclear, a doctor may order a blood test to measure follicle-stimulating hormone (FSH). FSH is a hormone produced by the brain that signals the ovaries to release an egg. As the ovaries slow down, FSH levels rise significantly. Elevated FSH, combined with low estrogen levels, supports a diagnosis of menopause or perimenopause.
A doctor may also check thyroid function, since thyroid disorders can mimic menopause symptoms such as fatigue, mood changes, and irregular periods. A bone density scan may be recommended to assess osteoporosis risk, especially in postmenopausal women.
Menopause Care and Treatment
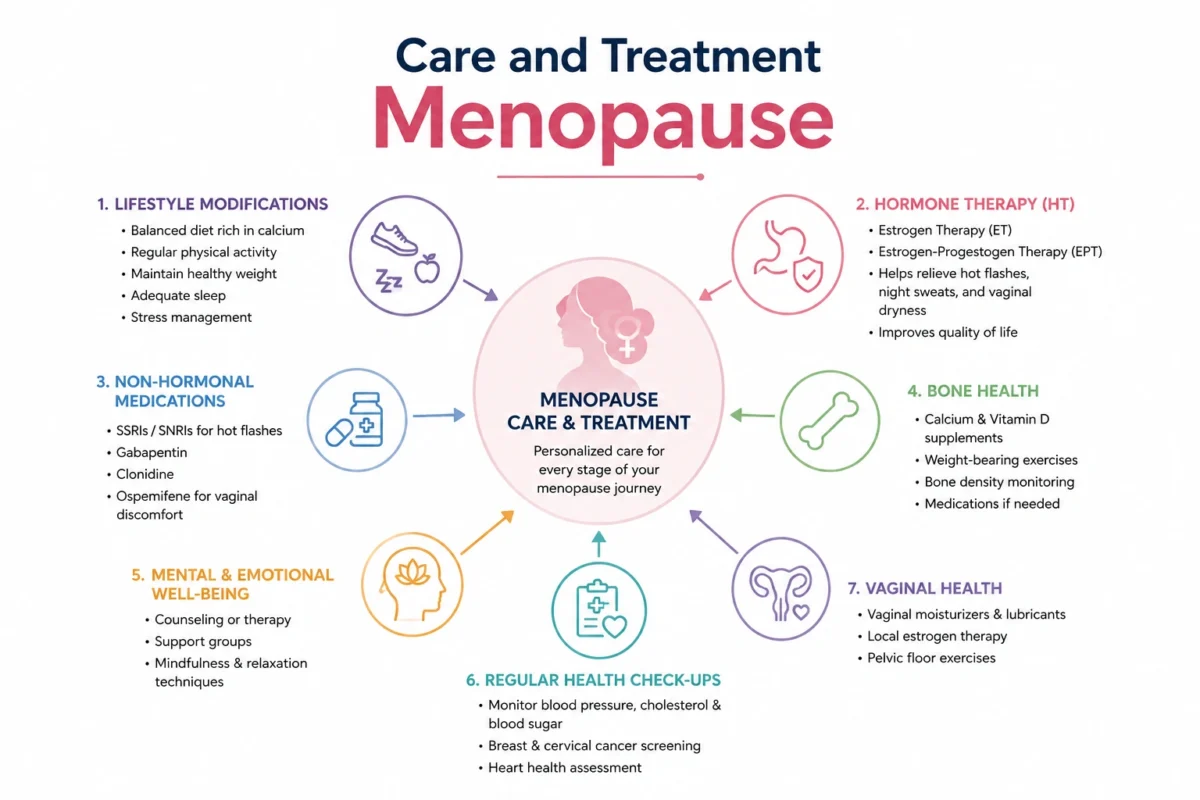
Home Care and Self-Care
Many women find meaningful relief through lifestyle changes. Dressing in layers, keeping a fan nearby, and sleeping in a cool room can all help manage hot flashes and night sweats. Regular aerobic exercise improves mood, supports bone strength, and helps maintain a healthy weight. A balanced diet rich in calcium and vitamin D supports bone health. Limiting alcohol, caffeine, and spicy foods may reduce hot flash frequency for some women. Mindfulness practices and stress management techniques, such as yoga and deep breathing, can ease anxiety and improve sleep.
Medical Treatment
For women with moderate to severe symptoms, several effective medical treatments are available. A doctor or specialist will help determine the most appropriate option based on individual health history.
Hormone therapy (HT): Replacing estrogen (and often progesterone) is the most effective treatment for hot flashes, night sweats, and vaginal dryness. It comes in pills, patches, creams, gels, and vaginal rings. The benefits and risks vary depending on a woman’s age, type of therapy, and medical history, so it must be discussed thoroughly with a doctor.
Non-hormonal prescription medications: Certain antidepressants and blood pressure medications have been found to reduce hot flash frequency in women who cannot or prefer not to use hormone therapy.
Vaginal estrogen: Low-dose estrogen applied directly to the vagina in cream, tablet, or ring form can relieve dryness and discomfort without significantly raising overall estrogen levels.
Bone-protecting medications: For women with low bone density, a doctor may prescribe medications that help maintain or rebuild bone strength.
Prevention and Management Tips
While menopause itself cannot be prevented, you can take proactive steps to protect your health and ease the transition:
Stay active: Aim for at least 150 minutes of moderate exercise per week. Weight-bearing exercises such as walking, dancing, or strength training are especially helpful for bone health.
Eat a bone-healthy diet: Include foods high in calcium (dairy, leafy greens, fortified foods) and vitamin D (fatty fish, fortified milk, sunlight exposure) to reduce the risk of osteoporosis.
Quit smoking: Smoking is linked to earlier menopause and more severe symptoms, as well as increased risk of heart disease and bone loss post-menopause.
Limit alcohol: Excessive alcohol can worsen hot flashes, disrupt sleep, and contribute to bone thinning.
Schedule regular health screenings: Bone density scans, cholesterol checks, and cardiovascular assessments become especially important during and after menopause.
Prioritize mental health: Talk to a counselor, join a support group, or speak to your doctor if mood changes or anxiety are affecting your quality of life.
When to See a Doctor
While menopause is a natural process, certain symptoms signal that you need medical attention promptly. Contact your doctor if you experience:
Vaginal bleeding after menopause (12 or more months without a period) this should always be evaluated, as it may indicate a more serious condition.
Extremely heavy or prolonged periods during perimenopause.
Hot flashes or night sweats so severe that they significantly disrupt sleep, work, or daily activities.
Symptoms of depression, including persistent sadness, loss of interest, or thoughts of self-harm.
Signs of a urinary tract infection, such as burning, urgency, or blood in the urine, which become more common after menopause.
Chest pain, shortness of breath, or signs of a heart problem, postmenopausal women have a higher risk of cardiovascular disease.
Menopause symptoms starting before age 40, which may indicate primary ovarian insufficiency or another condition needing evaluation.
Sudden or severe memory problems that go beyond typical forgetfulness.
A Final Note
Menopause is a significant life transition, but it does not have to be a silent or lonely one. Millions of women navigate it every year, and effective support — medical, emotional, and practical — is available. Please do not dismiss or ignore symptoms that are affecting your quality of life. Speak openly with your healthcare provider about what you are experiencing; together, you can create a management plan that works for your body and your life.
This article is published on Dcotiplus for informational purposes only and does not replace professional medical advice. Always consult a qualified healthcare provider for diagnosis and treatment.



