Decoding the Red Eye: Beyond Pink Eye
Red eye is a symptom, not a condition, and has at least eight common causes of red eye. Knowing key eye redness symptoms helps you determine whether you’re dealing with irritation, conjunctivitis, dry eye, or something more serious like uveitis. This article explores the main causes of red eye and gives you a clear comparison of pink eye vs red eye, so you can better understand your symptoms.
Redness means increased blood flow to the eye surface vessels. If you’re reading this, you’re likely wondering: Is my red eye pink eye, or something else? Start by symptom checking: when did the redness begin, is there pain, vision changes, discharge, or is just one eye affected? Use this guide to compare your symptoms to the most common red eye causes, understand the key differences between pink eye vs red eye, and recognize when to see a doctor.
Pink Eye vs Red Eye: What’s the Difference?
Pink eye, or conjunctivitis, is inflammation of the conjunctiva, the clear membrane lining the eye and eyelids. While conjunctivitis is common, remember that many other red eye causes, including dry eye and uveitis, can also produce similar eye redness symptoms. That’s why understanding pink eye vs red eye is important for anyone navigating these symptoms.
Conjunctivitis comes in three main subtypes. Viral conjunctivitis, the most common type, is usually linked to the same viruses that cause the common cold. Bacterial conjunctivitis produces thicker discharge and responds to antibiotic eye drops. Allergic conjunctivitis is triggered by allergens like pollen, dust, or pet dander and tends to affect both eyes simultaneously with significant itching.
Pink eye signs include watery or sticky discharge, itching, and both eyes being affected. If you have these symptoms, conjunctivitis is the likely red eye cause. Viral and bacterial forms are contagious through hand-to-eye contact. Most viral cases resolve in one to two weeks; bacterial cases clear faster with treatment. If your symptoms don’t match, keep reading. Dry eye, uveitis, or another condition might be responsible. This article will help you track your eye redness symptoms and guide you through what to do next.
Other Common Causes of a Red Eye
If your symptoms do not quite match the pink eye picture, one of the following red eye causes is likely responsible.
Dry Eye Syndrome
Dry eye is among the most common red eye causes in adults, particularly those over 40 and anyone who spends long hours on screens. When your eyes do not produce enough tears, or the tear film evaporates too quickly, the surface becomes irritated and inflamed. Dry eye can produce persistent eye redness symptoms like a gritty or burning sensation, and paradoxically, excessive tearing. Artificial tears and screen breaks help significantly in mild cases. You can find more on nutritional factors that affect eye moisture in our article on nutrient deficiencies and their health effects. Understanding whether your symptoms are due to dry eye, conjunctivitis, or another cause like uveitis will help guide your next steps.
Allergic Reactions
Seasonal allergens, dust mites, and pet dander can all trigger red eye as the immune system releases histamine in response. Both eyes are usually affected, and intense itching is the defining symptom that sets allergic red eye apart from other causes. Antihistamine eye drops and oral allergy medications manage most cases effectively.
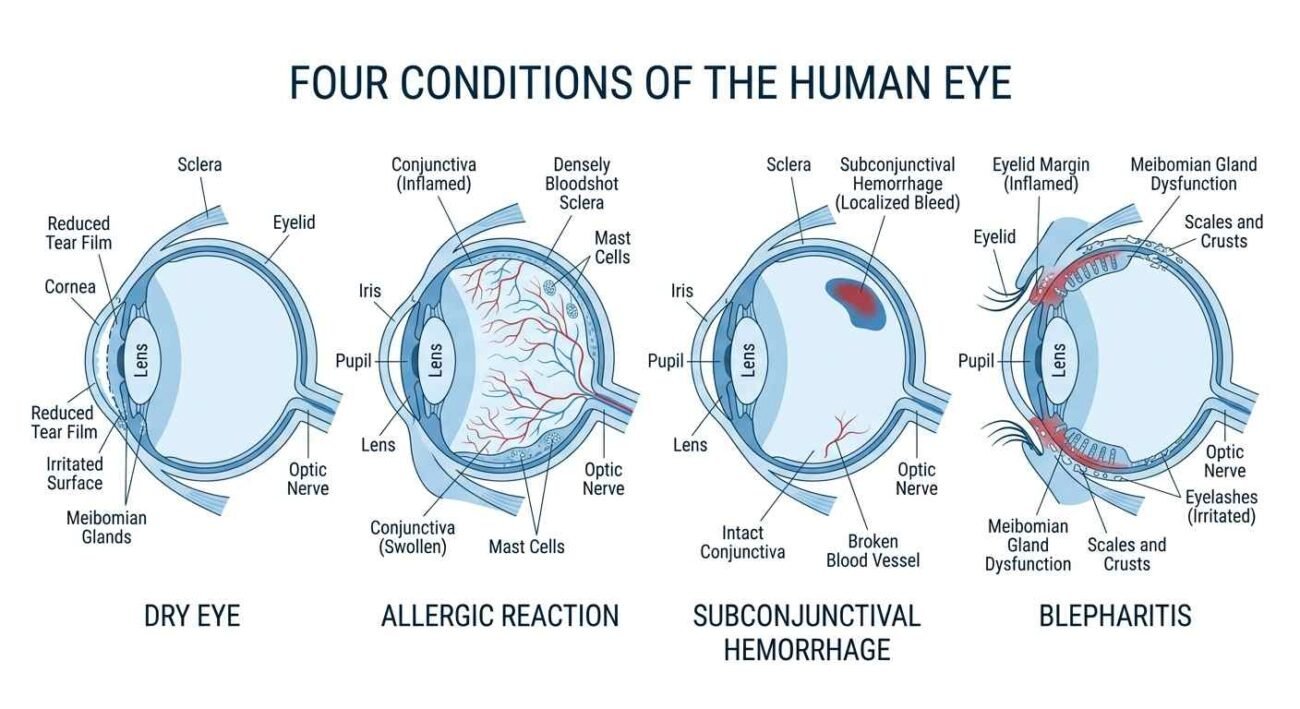
Subconjunctival Hemorrhage
This one looks alarming, but it is almost always harmless. A subconjunctival hemorrhage occurs when a tiny blood vessel beneath the conjunctiva breaks, causing a vivid red patch on the white of the eye. Straining, coughing, sneezing, or even rubbing the eye can trigger it. There is typically no pain, no discharge, and no vision change. Blepharitis is a long-term inflammation of the eyelid edges that often occurs due to a buildup of oils, bacteria, or skin debris at the base of the eyelashes, according to StatPearls. It produces redness along the eyelid edges, crusting, and a burning sensation. It tends to be a recurring condition rather than a one-off episode, and management involves regular warm compress application and careful eyelid hygiene rather than a single course of treatment.
Contact Lens Irritation or Overwear
Wearing contact lenses too long, improper cleaning, or overdue replacement irritates the eye. According to Oliver Schein, reduced corneal oxygen can cause corneal neovascularization and visible redness. Remove your lenses if you feel discomfort.
Foreign Object or Corneal Abrasion
Dust, an eyelash, or a corneal scratch will quickly redden your eye as it responds to the irritant. You’ll usually feel something in your eye. Rinse with clean water first. If the sensation or vision problems persist, see a doctor. An untreated corneal abrasion can become infected.
Uveitis
Uveitis is inflammation of the uvea, the middle layer of the eye that includes the iris, ciliary body, and choroid. Unlike surface-level red eye causes, uveitis involves deeper structures and can threaten vision if not treated. It often causes redness concentrated around the iris, light sensitivity, blurred vision, and significant eye pain. These are eye redness symptoms that should never be ignored. If you notice these symptoms, or if you’re uncertain whether you have conjunctivitis, dry eye, or uveitis, it’s safest to get checked by a doctor as soon as possible.
Acute Angle-Closure Glaucoma
Acute angle-closure glaucoma is the most serious cause of red eye and a medical emergency. It happens when fluid pressure spikes in the eye, damaging the optic nerve. Symptoms are sudden, severe eye pain, vision loss, halos around lights, nausea, and vomiting. Seek emergency care immediately. Delay can cause permanent vision loss.
Red-Flag Symptoms That Need Same-Day Care
Most red eyes are not emergencies, but certain symptoms demand urgent same-day medical attention. If these occur during your self-check, contact an eye doctor or seek emergency care immediately.
- Severe eye pain that does not ease with over-the-counter pain relief, especially pain that feels deep rather than on the surface
- Sudden vision loss or significant blurring in the affected eye that was not there before
- Extreme light sensitivity that makes opening your eyes in normal light painful
- A visible white or grey spot on the colored part of the eye, which may indicate a corneal ulcer
- Recent eye injury or chemical splash, even if it initially seems minor
- Halos around lights with nausea or vomiting signal acute glaucoma, which needs emergency care right away. Do not delay.
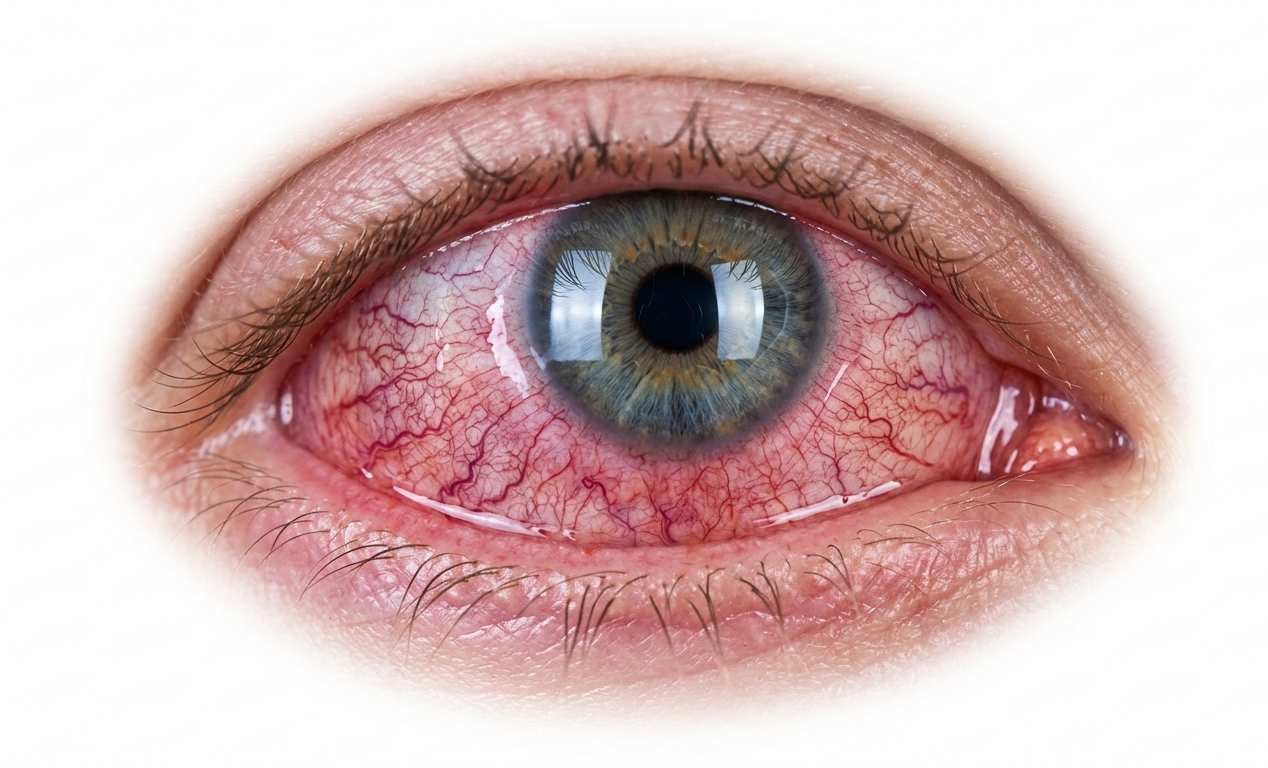
How Eye Doctors Diagnose the Cause
When you visit an eye doctor for a red eye, the examination is more systematic than it might appear. A slit lamp examination allows the doctor to view the eye under magnification and identify problems on the corneal surface, inside the anterior chamber, and along the eyelid margins. This single tool rules in or out the majority of red eye causes.
If a corneal scratch or abrasion is suspected, fluorescein dye is applied to the surface of the eye. The dye glows under a blue light and reveals any disruption in the corneal surface that would be invisible otherwise. For patients with eye pain or headache, intraocular pressure is measured to check for glaucoma. If a bacterial infection is likely, a swab of the discharge may be sent to a lab to identify the specific organism and guide antibiotic selection.
At-Home Care vs. Professional Treatment
| At-Home Care | When Professional Care Is Required |
| Cold compress to soothe irritation and reduce swelling | Any red-flag symptom listed above |
| Artificial tears for dryness and mild irritation | Symptoms that have not improved after 48 hours |
| Remove contact lenses at the first sign of discomfort | Contact lens wearers with worsening redness or pain |
| Antihistamine eye drops for known allergy-related redness | Visible spot or change on the cornea |
| Rinse with clean water if a foreign object is suspected | Eye injury, chemical exposure, or trauma of any kind |
| Rest and avoid touching or rubbing the eye | Fever accompanying the eye symptoms |
If your symptom check reveals only mild, recent-onset redness with no pain, no vision changes, and a clear cause (like screen fatigue or allergies), home care is reasonable. For anything outside that, or if you’re unsure, seeing an eye doctor is safest. It’s always better to err on the side of caution with red eye causes.
Prevention Tips
Protect your eyes with consistent habits. Once routine, they take little effort.
Wash your hands often, especially during cold and flu season. Don’t touch your eyes with unwashed hands—this spreads conjunctivitis. Replace contact lenses as your eye doctor recommends. Never sleep in daily-wear lenses; overnight wear raises corneal risk.
Wear protective eyewear for yard work, woodworking, or contact sports. The 20-20-20 rule recommends a 20-second break every 20 minutes of screen use, looking at something 20 feet away. Start antihistamines before peak pollen season if you have allergies; early action makes a difference. For more on environmental protection, see our guide on UV eye health.

According to Harvard Health Publishing, “dry eye syndrome is one of the most common causes of eye discomfort and is frequently mistaken for other conditions like pink eye. Once you explain what to look for, they can usually tell the difference themselves.”
Frequently Asked Questions
How can I tell if my red eye is contagious?
Viral and bacterial conjunctivitis are contagious; dry eye, allergic reactions, subconjunctival hemorrhage, and most other causes are not. If your redness came on after being around someone who was sick, if you have significant discharge, or if both eyes are affected, treat it as potentially contagious until a doctor tells you otherwise. Wash your hands often and avoid sharing towels or pillowcases.
Does pink eye go away on its own?
Viral conjunctivitis, the most common type, typically resolves on its own within one to two weeks without treatment. Bacterial conjunctivitis often clears faster with antibiotic drops, though mild cases may also resolve without medication. Allergic conjunctivitis will continue as long as the allergen is present, so treating the underlying allergy is essential. According to the American Optometric Association, stress can lead to symptoms like eyelid twitching and dryness, but it is not specifically identified as a cause of red eye.
Stress itself does not directly cause red eyes, but it contributes to conditions that do. Stress is associated with poor sleep, increased screen time, and suppressed immune function, all of which can trigger or worsen dry eye and make the eye more vulnerable to infection. According to a study published in BMC Ophthalmology, repetitive and prolonged eye rubbing can change the structure of the cornea and may lead to the development or worsening of keratoconus.
Not necessarily, but the pattern can be a useful clue. Pink eye often starts in one eye and spreads to the other. Dry eye and allergic reactions typically affect both eyes. Serious causes like uveitis, glaucoma, and corneal abrasions usually affect just one eye. One-sided redness with pain or vision change warrants faster attention than bilateral redness with itching and no other symptoms.
How long should I wait before seeing a doctor?
If you have any of the red-flag symptoms described above, do not wait at all. For mild redness with no pain and no vision changes, 48 hours of home care is a reasonable window. If things are not clearly improving by then, or if you are a contact lens wearer, book an appointment rather than continuing to wait.
Medical Disclaimer
This article is for informational purposes only and does not replace professional medical or dental advice, diagnosis, or treatment. Always consult a qualified healthcare provider with questions about your individual condition. Do not delay seeking medical attention because of something you read here.
References
- American Academy of Ophthalmology. Conjunctivitis: What Is Pink Eye? aao.org. https://www.aao.org/eye-health/diseases/pink-eye-conjunctivitis
DOI: Not applicable (organizational reference page) - American Academy of Ophthalmology. Red Eye Differential Diagnosis. aao.org. https://www.aao.org/eye-health/diseases/red-eye
DOI: Not applicable (organizational reference page) - Cleveland Clinic. Conjunctivitis (Pink Eye). my.clevelandclinic.org. https://my.clevelandclinic.org/health/diseases/8614-conjunctivitis-pink-eye
DOI: Not applicable (clinical reference page) - National Eye Institute. Pink Eye (Conjunctivitis). nei.nih.gov. https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/pink-eye
DOI: Not applicable (governmental reference page) - Azari AA, Barney NP. Conjunctivitis: A Systematic Review of Diagnosis and Treatment. JAMA. 2013;310(16):1721-1729.
DOI: 10.1001/jama.2013.280318 - Bhatt U, Lagnado R, Dua HS. Factitious keratoconjunctivitis and red eye presentations: a review. Eye. 2006;20(9):1027-1030.
DOI: 10.1038/sj.eye.6702103 - Leibowitz HM. The red eye. New England Journal of Medicine. 2000;343(5):345-351.
DOI: 10.1056/NEJM200008033430507



